Managing Arthritis – Movement & Other Tools
Arthritis is a term thrown around among medical professionals and everyday people alike, but what does it mean and how can we manage it? A glimpse into a recent talk given by Conveniently Active’s Rhiannon and me, Dr Ash Bowden: we’re going to discuss the challenges so many of us face with joint pain and stiffness and what ‘tools’ are available to us.
What is arthritis?

Arthritis (plural: arthritides) from the Greek ‘Arthron’ meaning joint and ‘-itis’ referring to a disease characterised by inflammation. It means ‘joint inflammation’ but can cause confusion around whether it’s a symptom or a disease itself.
Common features of arthritis include pain, swelling, stiffness and reduced range of motion. It is commonly used in place of conditions such as ‘osteoarthritis’ or ‘rheumatoid arthritis’ but to be accurate, ‘arthritis’ is a symptom/feature of an underlying disease and not a disease name itself.
This article looks at general ways to manage arthritis and not treatments specifically designed for a single condition. There will be lots of overlap with common conditions where arthritis is a key feature. These can include:
Osteoarthritis – the most common cause of arthritis. Once thought of only as wear and tear of the cartilage within a joint, it’s now understood to have a degree of whole joint inflammation also.
Autoimmune/Inflammatory Arthritis – the most common inflammatory arthritis is Rheumatoid Arthritis (RA) but hundreds of other autoimmune/inflammatory arthritides exist including psoriatic arthritis, ankylosing spondylitis, juvenile arthritis and more.
Metabolic Arthritis – this includes ‘Gout’ and ‘Pseudogout’ which can be linked to deposition of crystals in the joint space which cause inflammation.
Infective Arthritis – we may have experienced joint pain or aches with a viral illness, but some infections can specifically damage the joint space. Bacterial infection of a joint leading to ‘septic arthritis’ is deemed a medical emergency, something we’ll cover under “when to see a healthcare professional” at the end of this article.
Your management toolkit
The list of things we can do to help joint pain, stiffness and prevent worsening of symptoms is extensive. It ranges from lifestyle changes to individualised treatments and medication…
Exercise
Exercise is great for arthritis!
We recommend light to moderate intensity physical activity and exercise, aiming for a slow progression as you build strength, technique, and function. It’s important to acknowledge that pain may be a factor in normal activities so can be inevitable with exercise but finding movements that are associated with manageable periods of mild to moderately increased pain can be beneficial.
Exercise…
- Improves joint support by improving muscle strength around joints
- Improves flexibility, range of motion and reduces stiffness
- Improves posture
- Reduces pain associated with activities of daily living
- Improves balance and reduces risk of falls
Strength exercises can build strength and support around the sore, arthritic joints. Strengthening your muscles can take pressure off the sore joint surfaces. This can include body weight movements, using dumbbells, weight machines, pilates and reformer pilates, and mat work.
Incorporating stretching can help to improve mobility, flexibility and reduce stiffness. This can be done separately or part of pilates, yoga or before/after another exercise.
General physical activity is incredibly important to reduce our sedentary time. This avoids joint stiffness that we find worsens with longer periods of sitting or sleeping. General physical activity such as walking, gardening, group activities, help with healthy weight management also.
Low impact forms of exercise are helpful for arthritis:
- Swimming
- Aqua aerobics
- Walking
- Stretches
- Yoga
- Hydrotherapy
- Cycling
- Strength exercises
- Pilates
- Tai Chi
High impact or jarring exercises are typically avoided with arthritis.
Looking for an experienced and qualified guide to get you moving more and doing so safely? Contact Rhiannon from Conveniently Active to arrange a consultation with an Accredited Exercise Physiologist.
Website: https://www.convenientlyactive.com.au
Telephone: 0424 270 016
Nutrition
“The best diet for arthritis is a healthy, balanced diet. This can help you reach and maintain a healthy weight and reduce your risk of other health problems”
Arthritis Australia
There is very little evidence that specific foods influence arthritis. An exception to this is Gout where foods high in ‘purine’ (e.g. red meat, liver, kidneys, shellfish, sardines and mackerel) can trigger an attack.
Healthier dietary fats such as monounsaturated fat (e.g. vegetable oils, avocados, nuts and seeds) and omega-3 fats (e.g. oily fish, fish oil supplements and canola oil) are linked to reduced disease activity and inflammation.
Advice for nutrition management should be evidence-based, safe and accessible, and mostly comes down to simple, small changes that take time and consistency. We’re advise caution with ‘magic diets’ or very restrictive eating.
Weight Management
The goal of weight management to improve arthritis is reaching a ‘healthy weight’. This is important because:
- Being overweight increases stress on joints, particularly knees, hips and lower back. There’s a clear link between overweight populations and the risk of osteoarthritis.
- Being underweight can mean reduced muscle mass (sarcopaenia) which increases our risk of injury and joint function.
Simply put, weight management is about balancing the calories we eat with the calories we expend (TDEE, as explained below), which can be approximated using the Harris-Benedict formula.

The graphic above illustrates the TDEE, or Total Daily Energy Expenditure, which consists of the Resting Energy Expenditure (REE) and the Non-Resting Energy Expenditure (NREE). Here are the additional acronyms to help decode the graphic, and if you’re keen to learn more about this please reach out!
EAT = Exercise Activity Thermogenesis
NEAT = Non-Exercise Activity Thermogenesis
TEF = Thermogenic Effect of Food
BMR = Basal Metabolic Rate
EEE = Exercise Energy Expenditure
Weight management is evidently not easy though, otherwise it wouldn’t be the immense health problem and the contentious public issue that it is. With our diet we’re managing our hunger, our mental health, our social life and eating around busy lives all whilst maintaining a healthy relationship with food (dispelling the idea that foods can be ‘good’ or ‘bad’)
For safe and well-informed advice on nutrition and weight management we recommend seeing a qualified dietician. Contact Rhiannon or Ash for our trusted dietitian recommendations.
Medication
Medication can be very specific to the type and cause of arthritis as well as the individual, it’s important to seek informed individualised advice from your GP or specialist. This is a very brief section on the general principles of medication options for different types of arthritis.
Medication can be aimed at symptoms management (e.g. pain relief) or reduction of inflammation to reduce symptoms and disease progression. Due to the broad variety of arthritis, it’s very common to have some patients respond to some medications/treatments whilst others don’t.
Pain Relief
Pain relief can help to manage baseline pain that we experience with more significant arthritis and/or to manage pain exacerbations that occur from time to time. Over-the-counter options include paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen*. Beyond this, stronger or longer-lasting pain relief can be prescribed by your GP or specialist.
*It’s highly recommended to seek medical advice if using over-the-counter medication regularly or if considering prescription medications.
Inflammation Targeting
Some medications (e.g. NSAIDs) act as anti-inflammatories as well as pan relief so may be more effective for arthritis. Depending on the type of arthritis and the number of joints affected, local injections of steroids or tablet form steroids may help reduce inflammation, pain and joint stiffness.
Specialist Medication
If you’re referred to a specialist for management of your arthritis, you may have discussions about more specialist medications. These can include ‘Disease-Modifying Antirheumatic Drugs’ (DMARDs) or ‘Biologics’ such as methotrexate or infliximab respectively. These medications will be very patient and disease specific and may not be relevant for your condition – if in doubt, ask your GP for advice.

Acupuncture
Research offers limited although somewhat promising evidence that acupuncture (and dry needling) can help with arthritis symptoms. Acupuncture specifically is based on a concept of life energy called Qi (chee) that flows through the body along 20 invisible channels called ‘meridians’.
Study outcomes mostly note, if an improvement, it is with physical function and pain. A systematic review in ‘Evidence-based Complementary and Alternative Medicine’ deemed it “worth trying”.
Importantly, the negatives include that it can be very expensive, and that pain, bleeding and infection are all associated with needle use, as well as the rarer nerve injuries too.

Heat & Cold Therapies
The evidence is limited on the benefits of hot and cold therapy but both can be beneficial so they’re definitely worth a try!
Cold is typically great for helping to reduce heat and pain of a joint/area after more intense movement (e.g. after an exercise session) and can provide numbing pain relief.
Heat is great for feelings of joint stiffness or tightness as it helps to relax the muscle. This is especially good before movement during those colder winter days.
Massage
Massage can help to relieve pain, improve flexibility, reduce joint stiffness, work in conjunction with an exercise regimen and help with stress relief and sleep.
Key points when considering massage is that it may help with symptoms such as pain, flexibility and stiffness but can be very dependent on the type of arthritis, the massage therapist and your body. Massage can’t treat the underlying inflammation.
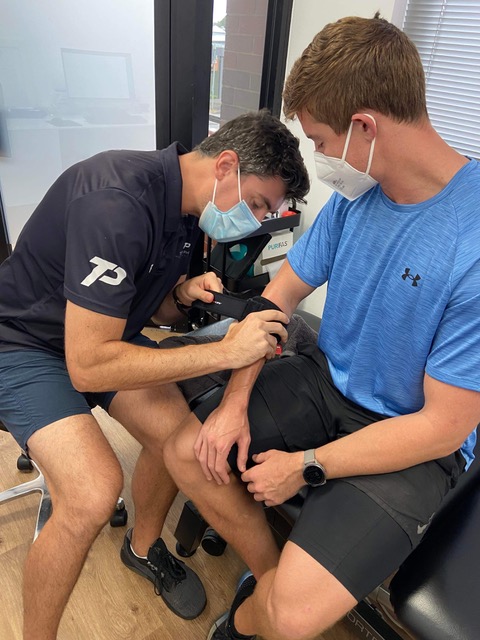
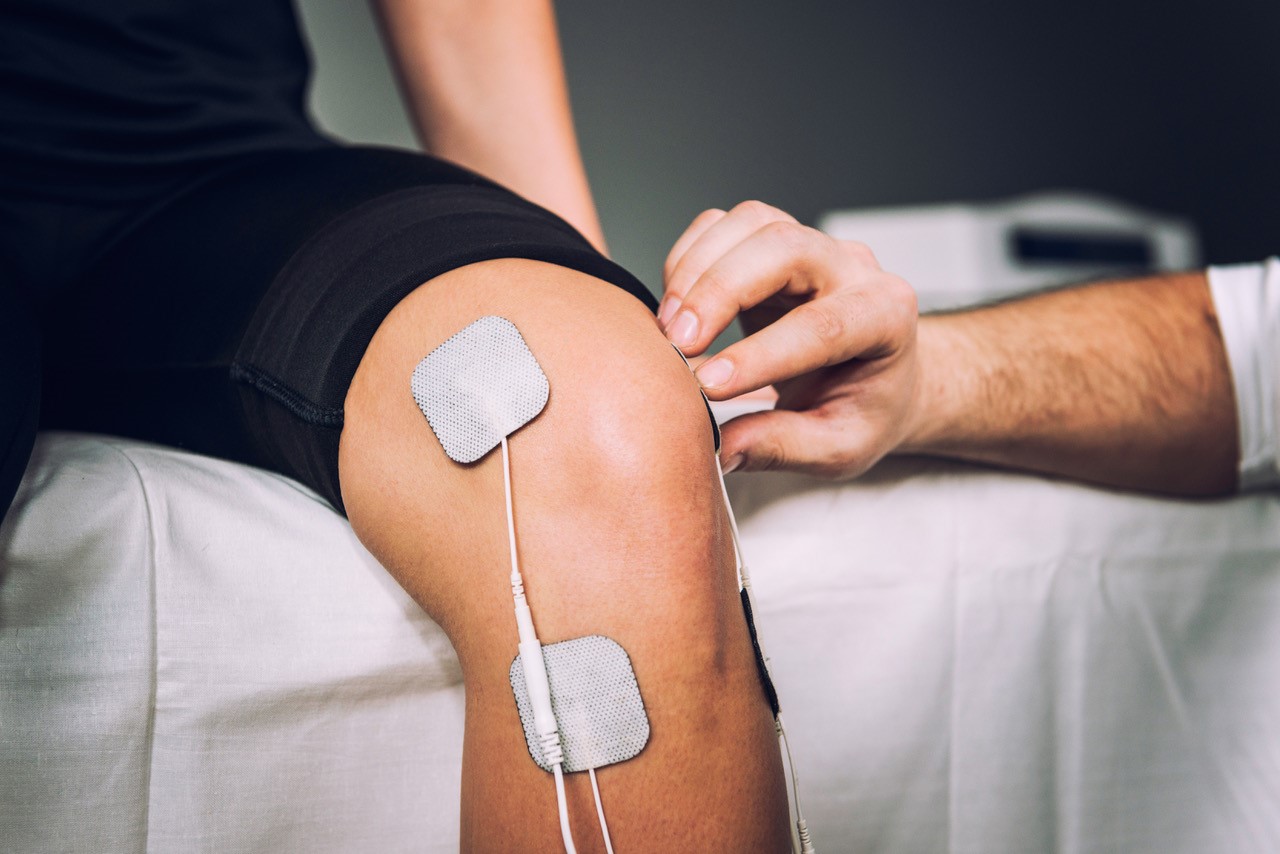
Electrical Nerve Stimulation
There are many different forms of electrical nerve stimulation (ENS) but the most common is ‘TENS’ (transcutaneous electrical nerve stimulation.) This uses sticky electrode patches attached to a battery-operated device aimed at overriding pain signals and triggering endorphins (our bodies natural painkillers). Current evidence suggests that TENS helps both short- and long-term pain management.
Other forms of ENS include neuromuscular electrostimulation, spinal cord stimulation and non-invasive interactive neurostimulation (NIN). Discussion with your GP and/or physiotherapist is important with this therapy, especially given the increasing online and unregulated market for products.
Relaxation Techniques
Depending on the severity of arthritis, pain can become quite debilitating, which can lead to increased rates of depression, anxiety, stress, and reduced sleep quality. Relaxation techniques can help to counteract this and include:
- Meditation
- Mindfulness
- Yoga
- Exercise
- Reading
- Art
- Socialising
- Knitting
Remember that what we find relaxing differs from person to person.
Supplements
The market for supplements is one of the fastest growing and least regulated, so we always advise caution and to discuss with your GP, healthcare professional or specialist if possible.
Two important cautionary notes:
1/ Supplements are often expensive for a very limited gain. We’ve included them at the bottom as there are much more effective tools to consider first but depending on the individual and budget, some supplements may prove beneficial.
2/ Some supplements can interact with other medications. A common example is a medication called Warfarin and its metabolism can be altered by a whole range of supplements: St John’s Wort, grapefruit juice and even…cocaine (hopefully no-one is using that to manage their arthritis!).
Omega-3 Oils are of the few supplements that have been shown to reduce inflammation, particularly in rheumatoid arthritis. This can be found in oily fish (sardines, salmon), linseed oil, canola oil and ready-made capsules.
Glucosamine & Chondroitin are both substances naturally produced by the body and found in cartilage so once thought to be beneficial to protect against and/or help arthritis. Unfortunately high-quality studies show little or no benefit for osteoarthritis.
Herbal supplements…the list is endless. A literature review looked at the impact of nine specific herbal supplements but beyond that, we strongly advise discussing these with your specialist. If they come with the promise of a miracle cure, please proceed with caution.
When to see a healthcare professional
If you’re suffering from an ongoing joint problem – this can be symptoms that last more than 3 days with no clear cause, several episodes of joint symptoms within a month or significant joint pain – we recommend booking an appointment with your GP and/or physiotherapist to have the problem assessed and consider further investigations. Early assessment can help prevent recurrence of symptoms and in some cases reduce progression of the disease.
If you’re wondering who can help improve your health during your arthritis journey, why not read “Meet Your Support Team”.
Importantly,
- If pain is unmanageable despite paracetamol and/or your prescribed pain relief
- If you could have an infected joint (e.g. it’s newly hot, red, swollen, painful +/- associated fevers)
- If you’re unable to safely function at home
Please call 000 or attend your nearest emergency department to see a doctor.
About the authors

Rhiannon Walton is an Accredited Exercise Physiologist who graduated from the University of Sydney in 2013 with experience working in private practice as well as hospital settings.
Rhiannon became an EP after having rehab on her knee since the young age of 9 years old due to recurrent patella dislocations and two major knee surgeries. Aged 31, she lives with high grade knee arthritis but manages extremely well with exercise along with other treatment strategies.
Dedicating her career to help others improve strength, mobility and confidence in movement, Rhiannon is driven to help with chronic pain, injuries and health conditions.

Dr Ash Bowden is an Emergency Doctor based on the Central Coast, passionate about improving health and happiness through physical activity. After a light-bulb moment on ward round with an Intensive Care Consultant in the UK, Ash dedicated his career to improving how active we can all be.
Ash has also created the Do More Activity Search Engine, a ‘Google for Exercise’, to empower everyone to find movement that suits them. The goal is to get our community more active. With increased physical activity we experience less pain, improved mental health, and improve our physical health. In the long run, fewer people will find themselves in hospital with preventable illnesses.
Disclaimer
The information and opinions expressed in this article are my own and not the advice of a local health district or governing body. Information has been collected from reputable sources at the time of writing. Always seek the guidance of your doctor with any questions regarding your own health or a medical condition.
By Dr Ash Bowden – For more information on keeping active visit https://do-more.live
Facebook: Dr Ash Bowden | Instagram: @doctordomore